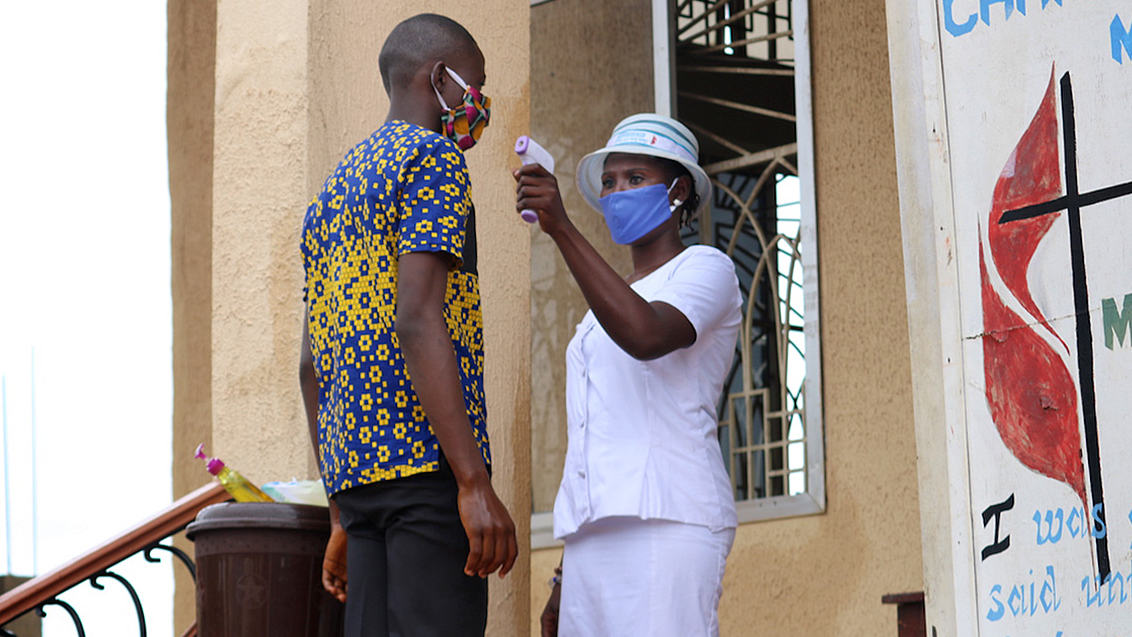
Health officials across Africa are struggling to contain the COVID-19 pandemic, despite lessons learned in the fight against Ebola.
As with the 2014 Ebola outbreak in West Africa, they are striving to overcome public skepticism and other barriers, but they are also wiser.
“Our experience with Ebola has prepared us to handle the coronavirus pandemic,” said Dr. Francis Kateh, chief medical officer of Liberia and a United Methodist. Although government efforts to warn citizens are disputed by COVID-19 skeptics, he said, most people take lessons learned from Ebola as a warning.
However, Liberia and other countries have not received the level of support that they did during the Ebola outbreak of 2014 and 2015.
“International support to fight COVID-19 is very thin,” he said. “Citizens have to be very careful to avoid the deaths that come as a result of this pandemic.”
Liberia and Sierra Leone were among the hardest-hit countries during the Ebola epidemic, and Congo continues to struggle with outbreaks. While officials say they are applying what they learned from fighting Ebola, their countries — and the continent — are overwhelmed. The more contagious delta variant and lack of vaccines have made this battle more difficult.
“This strain is serious and is killing more people,” said Dr. Austin Demby, Sierra Leone health minister. “The combination of a highly transmissible virus, more people hospitalized and more dying is extremely concerning.”
Initially, Africa appeared unscathed by COVID-19, recording fewer infections and deaths than China, Europe and the Americas. But in mid-July, the World Health Organization reported a sharp rise in COVID-19 deaths in Africa. With an unstable health infrastructure, no vaccines yet produced on the continent and limited pandemic experts, Africans are challenged with garnering adequate resources to contain the disease.
“Deaths have climbed steeply for the past five weeks. This is a clear warning sign that hospitals in the most impacted countries are reaching a breaking point,” said Dr. Matshidiso Moeti, WHO Regional Director for Africa, in a July 15 release.
“Under-resourced health systems in countries are facing dire shortages of the health workers, supplies, equipment and infrastructure needed to provide care to severely ill COVID-19 patients,” he said.
Unlike the West African Ebola outbreak, when synergy existed between government and faith leaders, the fight against COVID-19 in Sierra Leone has been mainly government-centered.
In a July 6 press statement, the Council of Churches in Sierra Leone, of which The United Methodist Church is a member, expressed dissatisfaction over President Julius Maada Bio’s July 1 nationwide broadcast in which he suspended congregational worship, among other measures, to contain the third wave of COVID-19, without conferring with faith leaders. On Aug. 16, the ban was lifted, but churches must adhere to guidelines, including the use of face masks, social distancing and limiting services to 90 minutes.
When Ebola broke out in 2014, governments were initially slow to respond. The delay, combined with skepticism in the public, led to a rapid spread from Guinea to Sierra Leone and Liberia. Governments turned to faith leaders for messaging help.
The bishops in Sierra Leone and Liberia worked with United Methodist Communications on developing SMS networks for pushing out information about healthy preventive practices and offering encouraging pastoral messages.
Now, the Sierra Leone Conference has no team or logistics in place to provide a robust COVID-19 response, especially with the 2020 death of Bishop John K. Yambasu, who led the Ebola response at conference and church-wide levels, said the Rev. Solomon Rogers, administrative assistant to interim Bishop Warner Brown. Yambasu also was a key figure in the national campaign against Ebola.
“A few departments and units are responding in some way. But there is no annual conference COVID-19 response team as we had in Ebola,” Rogers said.
According to the Africa Centres for Disease Control, only 1.7% of the population in Africa — about 24 million people —have been fully vaccinated, the BBC reports.
Demby urged all Sierra Leoneans to take available vaccines. He noted that Sierra Leone vaccine intake was among the lowest in West Africa — only 225,380 vaccine doses administered as of Aug. 16, according to data gathered by Reuters. That represents about 1.4% of the country’s population of 7 million.
The quantities of AstraZeneca and Sinopharm vaccines that were donated to the government are limited.
“Sierra Leone does not have the luxury to choose among several available vaccines,” Demby said. “We have only two, so we must take them.”
